Metabolic Adaptations to Pregnancy
High adiposity at birth is associated with poor metabolic outcomes and increased risk of obesity in childhood and adult life. Maternal obesity is associated with increased fetal adiposity, but not all obese patients have obese babies. Maternal insulin sensitivity is a key predictor of fetal fat accrual, but the mechanisms regulating insulin signaling during pregnancy are unknown. Insulin sensitivity improves 120% following delivery of the placenta, suggesting a placental factor may regulate insulin signaling during pregnancy. As placental growth and gene expression is sensitive to maternal insulin levels in early pregnancy, and correlated to adiposity at birth, we propose that maternal-placental crosstalk is key to fetal growth regulation.
Placental-derived microRNAs (miRNA) regulate post-transcriptional gene expression in maternal tissues, and are detectable in maternal plasma throughout pregnancy. Thus, miRNAs may provide both a mechanism for maternal-placental crosstalk, and novel indicators of women at risk of high fetal fat accretion.
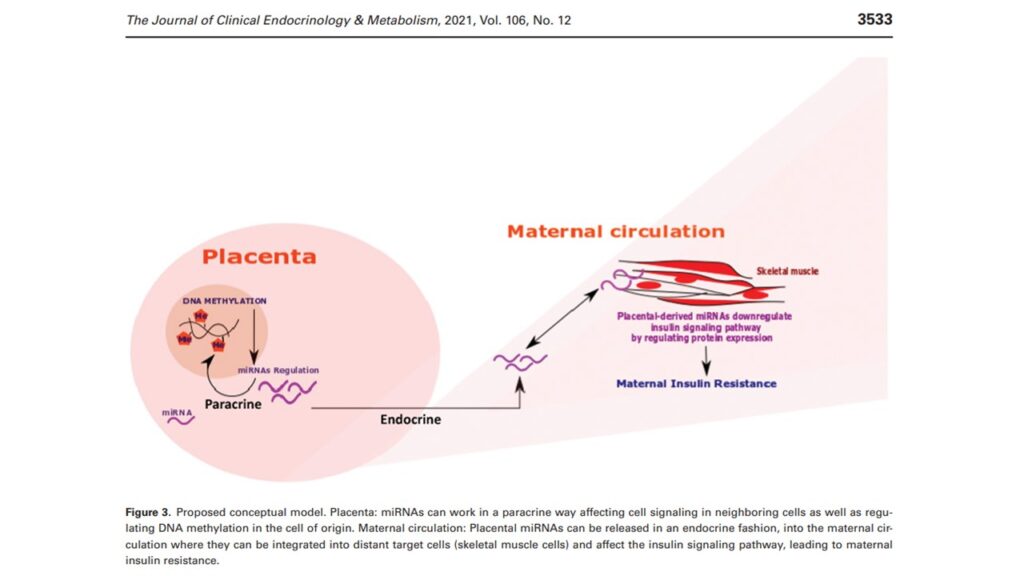
The overall goal of this study is to identify placental miRNA expression profiles associated with alterations in maternal insulin resistance (IR) throughout pregnancy resulting in high neonatal adiposity. We have found specific miRNA produced in the placenta that are associated with maternal insulin sensitivity (Alvarado et al, 2021). We are currently working on determining the paracrine and endocrine mechanisms underlying these relationships.
Stress sensing
The placenta is very sensitive to the maternal environment and may play a critical role in the translation of environmental stressors to pregnancy outcomes. In a study of over 120 pregnant patients, we identified fifteen miRNAs that were more highly expressed in the placentas of non-Hispanic Black (NHB) people. Several of these miRNAs were associated with cellular stress response pathways, suggesting that they may be responding to environmental stressors. Placental miR-192-5p expression was lower among NHB people and was positively associated with neonatal adiposity, suggesting it may be sensitive to structural racism with potential impacts on fetal growth.
Future studies will seek to determine the relationships between maternal experiences of racism and chronic stress with expression of these placental “stress sensors” and their potential role in placental function and fetal growth outcomes.
